Ultra processed foods (UPFs) increased mortality risk from chronic respiratory diseases (CRDs) in a large study of ~100,000 people in the United States.
Diets high in UPFs and dietary inflammatory index increased the risk of mortality from CRDs, including COPD and lung cancer. Healthy diets rich in antioxidants reduced the risk of death from CRD overall and COPD, which may be due to effects on inflammatory potential, although the impact of UPFs was not offset.


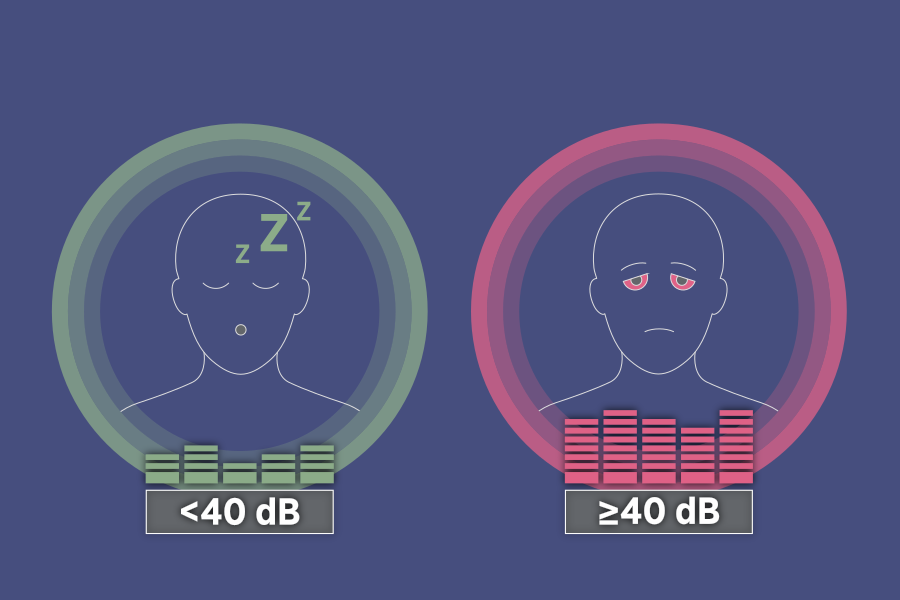
Noise during nighttime has a disruptive effect on sleep quality in individuals with COPD and increases their risk of acute exacerbations.
A study involving 518 people in China with COPD found that exposure to high noise levels (≥40 dB) during nighttime sleep hours significantly increased the likelihood of escalated therapy and urgent hospitalization for COPD exacerbations. This was up to twice as high compared with people experiencing lower noise levels.
The largest study of e-cigarettes and health outcomes to date, the All of Us research program in over 249,000 individuals in the United States, has shone new light on the cardiometabolic consequences of exclusive use of e-cigarettes.
Exclusive use of e-cigarettes significantly increased the risk of COPD by over 2-fold compared with non-use. However, it was not associated with hypertension, type 2 diabetes, heart failure or atherosclerotic cardiovascular disease.
The prevalence of asthma is high in people with type 2 diabetes and is not explained just by BMI, which is an important risk factor for both conditions.
A study of over 25,000 adults in Sweden found a 47% higher prevalence of current asthma among individuals with type 2 diabetes, even after adjusting for BMI, as well as other demographic and socioeconomic factors. Brothers and sisters with asthma were at increased odds of type 2 diabetes, indicating shared familial genetic and environmental risk factors.
.png)
A Global Working Group of experts across 40 countries has developed a blueprint in a first comprehensive study for the identification and management of cardiopulmonary risk in patients with COPD.
The experts call for improved cardiopulmonary risk identification and stratification in COPD as well as clinical pathways and integrated models for identifying comorbid COPD and cardiovascular disease. There is also a call to action for novel therapies and defining optimal management strategies.


Eating fast food 3 times a week or more increased emergency department visits for asthma in a large study of over 11,500 adults with asthma in California, United States.
Irrespective of BMI, an improved diet by reducing fast food consumption and increasing fruit and vegetable intake may be beneficial for adults with asthma and result in fewer emergency department visits due to asthma.

Airborne microplastics and nanoplastics originate from a variety of sources including roadside dust and domestic waste and can induce inflammation and oxidative stress when inhaled, ingested or on contact with skin.
Global distribution of these particulate plastics through the atmosphere poses significant health risks, especially when present in particulate matter and in urban areas, according to researchers from Taiwan. Mitigation strategies such as advanced oxidation processes and bioremediation alongside public health policies are needed to counter these adverse effects.

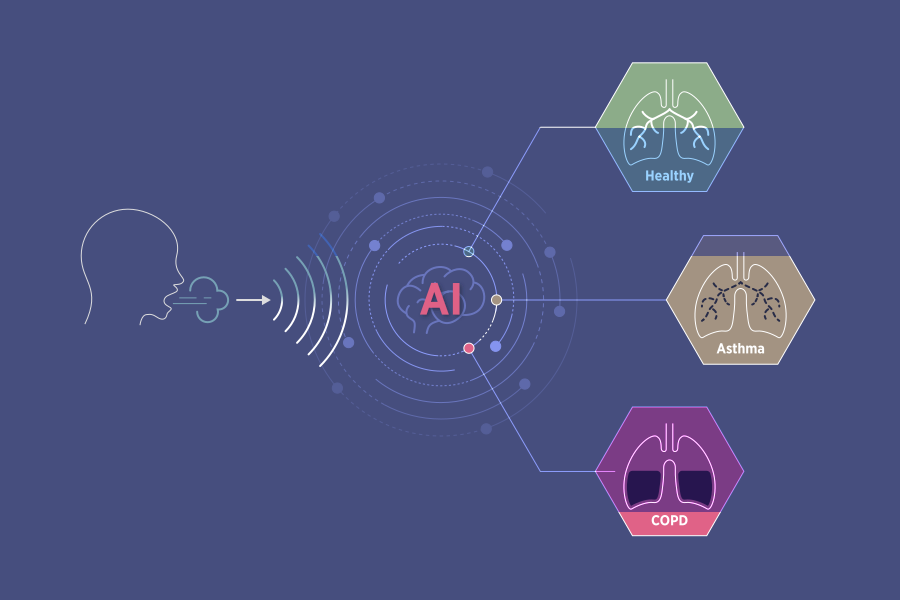
A novel AI model using dual-sound analysis shows strong potential to improve diagnostic practices in asthma and COPD management.
When differentiating between asthma and normal cases, the automated, lightweight model achieved 83% and 94% accuracy of cough and respiratory sounds, respectively. This international study suggests that advancements in AI-based detection of respiratory diseases may be beneficial to clinicians and respiratory healthcare professionals globally.
Despite improvements, COPD remains a significant health issue internationally, with older adults, men and people exposed to tobacco and pollution predicted to be particularly affected by 2050.
Based on data from the Global Burden of Disease 2021 study, analysis of the COPD burden in the Original BRICS countries between 1990 and 2021 showed reduced incidence, mortality and disability-adjusted life years overall, although there were gender and age disparities. Targeted COPD monitoring, assessment and management strategies remain important to reduce COPD burden in these countries.

In a UK study of over 134,000 women of reproductive age with asthma, the progestogen-only pill (POP) increased asthma attacks in certain asthma phenotypes.
Overall, there was no association between asthma attacks and combined oral contraceptive or POP use. However, POPs were linked to increased asthma attacks in women under 35, those with eosinophilic asthma and women with lower corticosteroid use, suggesting personalized approaches to contraception choices should be considered.

Asthma, COPD and interstitial lung disease (ILD) affect over 10 million people in the United Kingdom, often with poor respiratory outcomes.
This unique study using harmonized healthcare records from all 4 UK nations over 20 years reported an increased incidence of ILD in England, Wales, Scotland and Northern Ireland, but an overall decrease in asthma. COPD incidence, however, only decreased in England and Wales.

Asthma management was improved and emergency department visits reduced in a respiratory therapist–led community programme in California, United States.
An interdisciplinary approach incorporating home visits and educational modules, integrating clinical care with environmental and social factors, addressed some of the challenges in underserved communities and the management of chronic respiratory conditions.

CC-MED-2-03/2026






Διαμοιρασμός περιεχομένου