The impact of indoor air pollutants such as mould, cleaning agents and volatile organic compounds on asthma has been highlighted by the European Academy of Allergy and Clinical Immunology (EAACI).
The risk of new-onset asthma can be increased and asthma symptoms worsened by these common pollutants. The EAACI recommends including stricter regulations to protect vulnerable populations and incorporating exposure assessments into asthma management.
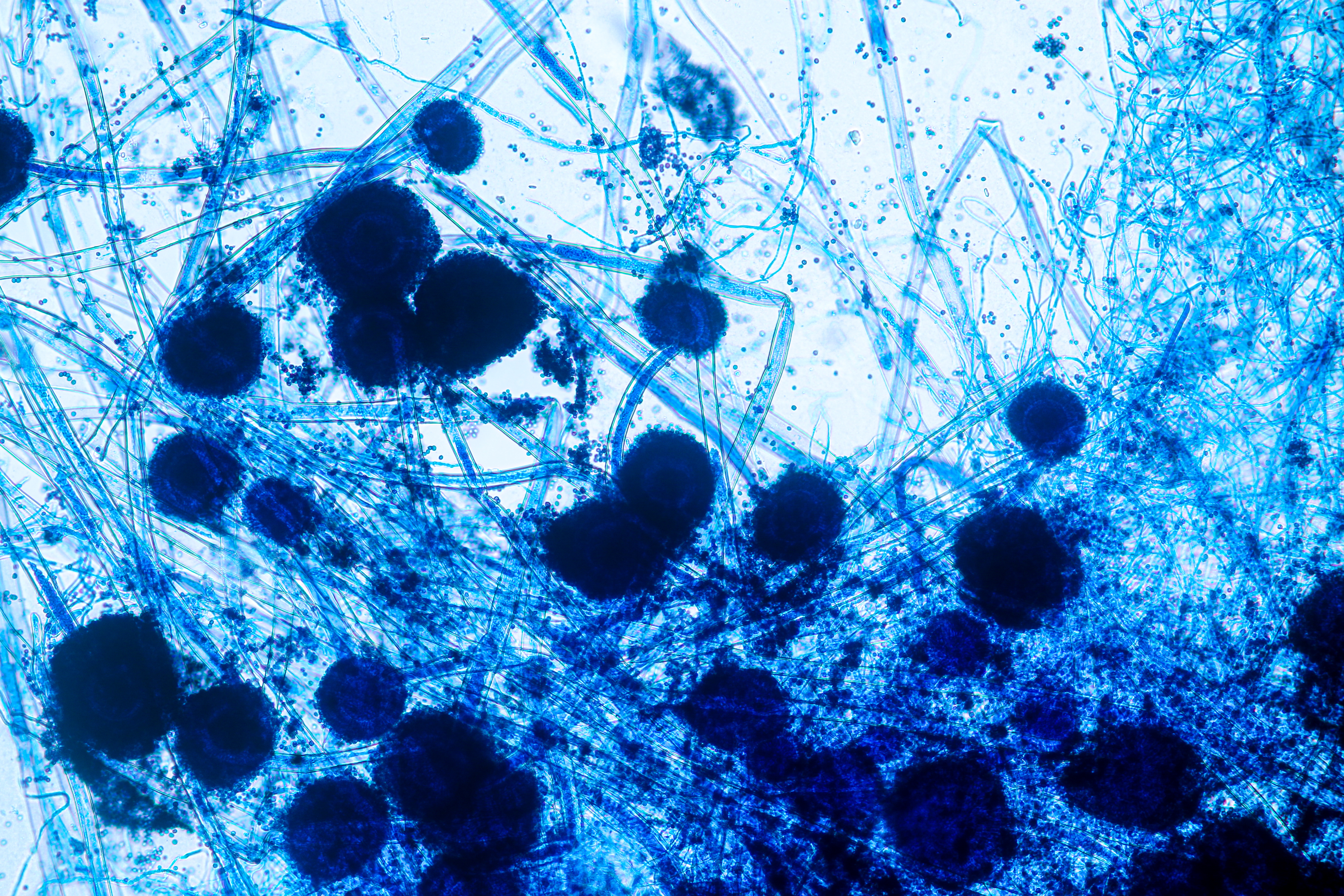
Asthma and atopic dermatitis are expected to rise to 275 and 148 million cases, respectively, by 2050, according to the Global Burden of Disease Study 2021.
This growth is partly driven by different risk factors in high- and low-income countries. High BMI is an important contributor to asthma globally, especially in high-income countries. In low-income settings, smoking and asthmagens have greater impact in asthma, and challenges such as limited resources are on-going for atopic dermatitis management.
Clinical remission of mild-to-moderate asthma is obtainable and sustainable.
The concept of clinical remission in asthma was first presented in 2020 and has since been assessed mainly in severe asthma. This study in patients in Japan revealed a considerably higher clinical remission rate in patients with mild-to-moderate asthma, although nearly 27% did not achieve remission.

A survey in the United Kingdom has given insights into patient experiences of asthma attacks and behaviours known to contribute to asthma deaths.
Almost two-thirds of patients did not fully understand what asthma attacks are or how to manage them. In some cases, this was linked to difficulties in recognizing attacks and delays in seeking help. The survey also found variations in self-management, which was influenced by the patients’ own experiences and their care.

Improved use of an educational tool for COPD in the United States showed benefits for education and hospital readmissions.
The ‘Green Light to Go’ tool educates patients on managing their COPD symptoms at home. An initiative to standardize its use in hospitalized veterans showed improvements in education of up to 100% and a decrease in the readmission rate of 5%.
.png)
The Global Burden of Disease Study 2021 revealed complex regional patterns of the burden of asthma due to NO₂ pollution.
The patterns were influenced by pollution control measures and economic development in low- and middle-income regions, and the burden of asthma increased with accelerated industrialization. Air quality measures have decreased concentrations of key pollutants like NO2 but the lack of significant reductions in asthma burden suggests other factors are at play.
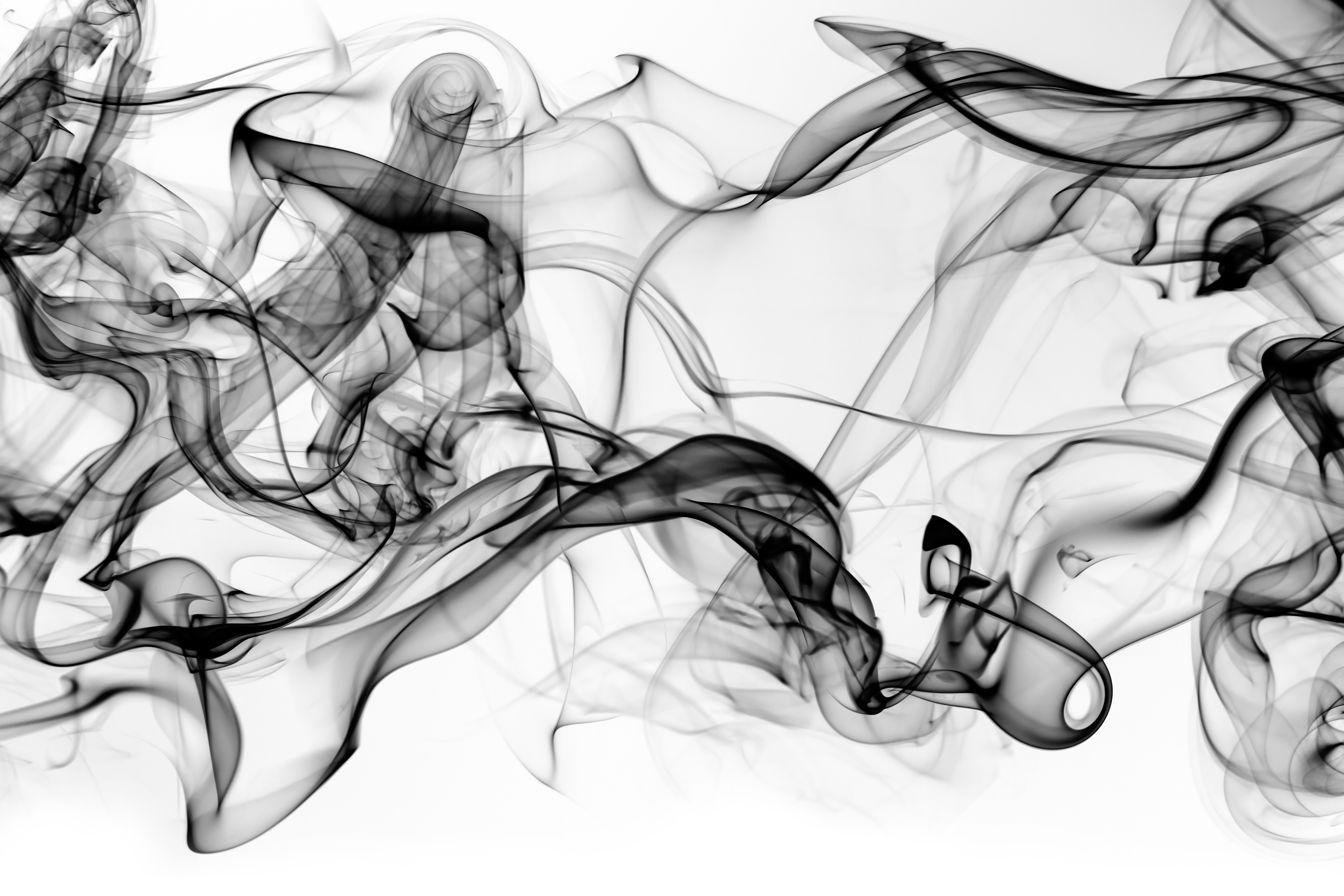
Bariatric surgery improved asthma control and decreased asthma exacerbation rates in a large study in France involving over 5000 patients.
Bariatric surgery in patients with asthma and obesity significantly improved asthma control 2 years after surgery. As well as improving asthma, bariatric surgery decreased healthcare utilization such as physician visits and asthma-related hospitalizations.
Green spaces affect respiratory symptoms differently in children and adolescents with asthma compared with adults with asthma.
In a study from an area of 400,000 inhabitants in Brazil, greenness was associated with uncontrolled asthma symptoms in over 300 children and adolescents, whereas for nearly 1000 adults the frequency of uncontrolled asthma was lower.


Asthma may be exacerbated by workplace environments in up to 1.5 million adults in the United States.
High asthma rates were reported in a broad range of industries and job roles. Identifying occupational triggers is important to implement targeted treatment strategies and help address asthma disparities.

Despite cognitive impairment being a common comorbidity in COPD, only a minority of physicians in Saudi Arabia have received adequate training on its management.
In a survey of over 800 physicians, most recognized that cognitive impairment leads to patients underestimating COPD severity and impacts self-management. However, alongside inadequate training, factors such as lack of standardized procedures contribute to suboptimal management of cognitive impairment in COPD.

An interactive pulmonary rehabilitation (PR) smartphone app improves symptoms and exercise capacity in patients with COPD.
In a study in Germany and Switzerland, outcomes in patients with COPD who use the app were similar to those receiving enhanced standard of care, highlighting its potential. Exercise capacity was improved in adherent users, suggesting that accessing the app might be valuable for patients who cannot access PR in person.

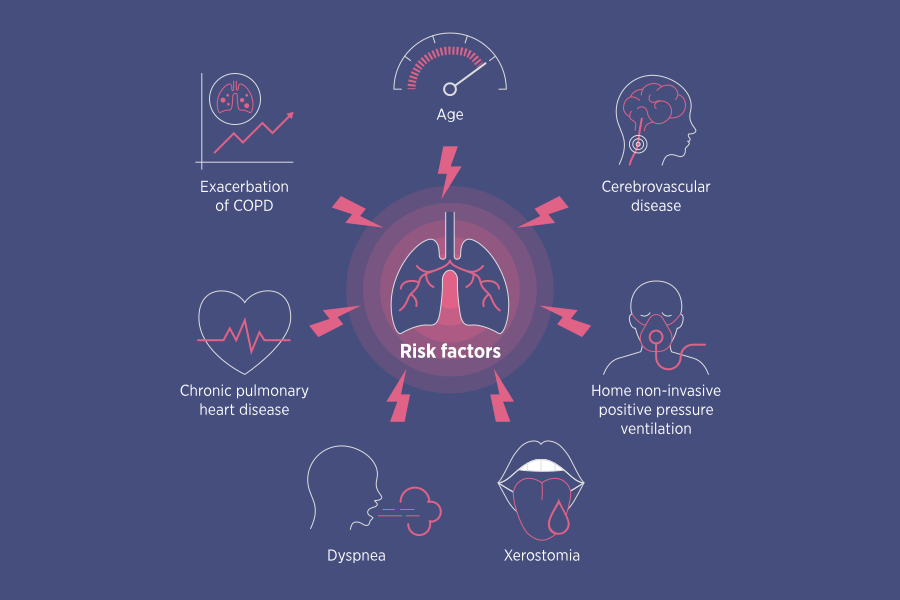
An innovative model to predict the risk of dysphagia in patients with COPD has been developed in China.
The risk prediction model used traditional factors known to cause dysphagia in COPD and incorporated several new ones. The model has the potential to be used for screening, detection and management of dysphagia.
Research in Indonesia suggests that AI shows potential as an educational tool for asthma, but improvements are needed.
ChatGPT was fully (100%) accurate for conveying information on etiology and pathophysiology but less so (70%) for medication-related responses. Of the latter, 12% were critically flawed and could potentially mislead users.
Inadequate access to safe and nutritious food, known as food insecurity, has been linked to respiratory health in the United States.
High food insecurity was reported for 20% of children and 14% of adults in National Health and Nutritional Examination Surveys (NHANES) data from 2007 to 2012. It was associated with increased asthma and wheezing particularly in women and non-Hispanic White people.

CC-MED-1-03/2026






Διαμοιρασμός περιεχομένου